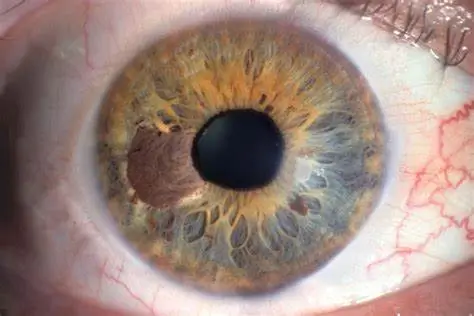
Immunotherapy treatment discovered that can have long-term survival benefit for Uveal melanoma
At CTRT, we are dedicated to finding better ways of treating cancer, as well as detecting, monitoring and understanding how cancer develops, particularly in rare cancers that don’t receive research funding elsewhere.
One of our trustees, Professor Paul Nathan has led a clinical trial at the Mount Vernon Cancer Centre, and has discovered a more successful way of treating Uveal melanoma.
Uveal melanoma is a rare, but often high risk, type of cancer of the eye that frequently spreads to other parts of the body (particularly the liver). Unlike skin melanoma, once the cancer has spread, it does not respond very well to so-called immune checkpoint inhibitors, a type of cancer treatment that uses the body’s own immune system to recognize and fight off cancer cells. However, data from the clinical trial led by Professor Paul Nathan at the Mount Vernon Cancer Centre indicated that another type of immunotherapy can have long-term survival benefit in patients with metastatic uveal melanoma, a form of the disease that has spread.
The immunotherapy used in the trial, tebentafusp, works by bringing cells of the immune system close to the melanoma cells, effectively directing the immune cells to kill the cancer cells. Tebentafusp can perform this bridging role because it was designed as a ‘bispecific fusion protein’, which means that it latches on to pieces of a particular protein that melanoma cells have in abundance on their surface, as well as to a protein called CD3, that is present on T cells, a type of immune cell that is particularly efficient at killing cancer cells.
Initial reports showed that, at 1 year, tebentafusp improved the survival of patients with metastatic uveal melanoma, and the latest trial results which have been published recently in the New England Journal of Medicine, showed that the benefit is still seen at 3 years.

Nearly 400 patients, all of whom had previously untreated metastatic uveal melanoma, took part in the trial. They were randomly assigned to receive either tebentafusp or another treatment — a checkpoint inhibitor (pembrolizumab or ipilimumab) or chemotherapy (dacarbazine). At 3 years, more of the patients who had been given tebentafusp were still alive (27%) compared with the patients receiving any of the other treatments (18%). The side effects of tebentafusp were similar to those seen previously which included a rash, fever/chills, itching and low blood pressure. Very few patients receiving any of the drugs had to stop treatment, and there were no treatment-related deaths during the trial.
Tebentafusp clearly presents an advantage over current treatments for Uveal melanoma but unfortunately, it does not offer a cure at present. Moreover, tebentafusp only works in a subset of patients — making broadening tebentafusp’s potential benefit another priority.
Nevertheless, the future for tebentafusp, perhaps in combination with other treatments, looks very promising. Professor Nathan is leading an international trial due to begin in summer 2024 that will look at whether tebentafusp, if given after the primary treatment to tackle the melanoma in the eye, can reduce the number of patients who relapse with metastatic disease. This clinical trial will take place at many centres throughout Europe and North America and is being run by the European Organisation for Research and Treatment of Cancer.
The trial was run and funded by Immunocore, with some staffing costs at Mount Vernon Hospital supported by CTRT.
The Cancer Treatment and Research Trust continues to support Professor Nathan’s research thanks to your generosity. You can donate towards our melanoma research here
Research paper published in the New England Journal December 2023: Hassel, J.C. Three-year overall survival with tebentafusp in metastatic uveal melanoma. N Engl J Med. 2023 Dec 14;389(24):2256-2266. doi: 10.1056/NEJMoa2304753.
Relates Posts
New Guidelines for Gestational Trophoblastic Disease
Gestational trophoblastic disease (GTD) comprises a rare group of pregnancy-related tumours, ranging from premalignant forms, including partial and complete hydatidiform moles (molar pregnancies), to malignant types (referred to as gestational trophoblastic neoplasia (GTN)), which include invasive mole, choriocarcinoma, placental site trophoblastic tumours and epithelioid trophoblastic tumours. Although uncommon, GTD affects around 220,000 women globally each year, with 22,000 developing GTN.
In a recent podcast, the Editor-in-Chief of the International Journal of Gynecological Cancer, Dr Pedro Ramirez, sat down with CTRT’s Chair of Trustee’s Professor Michael Seckl and Dr Christianne Lok, two leading international experts in gynaecologic oncology, to discuss Practical Guidelines for the Treatment of GTD: Collaboration of the European Organization for the Treatment of Trophoblastic Disease (EOTTD)-European Society of Gynecologic Oncology (ESGO)-Gynecologic Cancer Intergroup (GCIG)-International Society for the Study of Trophoblastic Diseases (ISSTD), recently published in the Journal of Clinical Oncology. Developed by 53 specialists across 31 countries, these guidelines represent the most comprehensive global consensus to date.
One key topic of discussion in the podcast was the importance of specialized GTD centres. The new guidelines define clear criteria for such centres, with the hope of improving access to expert care worldwide. Even though these tumours are uncommon, centralization of care, the experts explained, improves outcome, as shown in studies of other cancers and rare diseases.
The experts also emphasized that careful history-taking should always be part of the diagnostic process, regardless of any latest developments. Abnormal bleeding, severe nausea or abdominal pain can point to GTD, but confirmation relies on ultrasonography, measurement of human chorionic gonadotropin (hCG; a pregnancy hormone often raised in GTD), and most importantly, tissue analysis; genetic testing can also help. The guidelines also include flowcharts to guide doctors through diagnostic dilemmas.
Another focus of the guidelines is treatment approaches. For low-risk GTN, single-agent chemotherapy with either methotrexate or actinomycin D is highly effective; the choice of drug often depends on local healthcare systems and patient preference. For high- and ultra-high-risk patients, low-dose induction regimens are often advised prior to more intensive combination chemotherapy treatment to avoid dangerous complications. The experts highlighted how immunotherapy has emerged as a transformative treatment option, particularly for patients who previously faced poor outcomes, as well as offering new hope for patients with very rare subtypes such as placental site and epithelioid trophoblastic tumours.
Finally, the guidelines emphasize individualized follow-up. The accompanying flowcharts help clinicians tailor surveillance, while recent evidence has suggested that follow-up after partial and complete moles could potentially be shortened once hCG levels normalize — welcome news for women hoping to conceive again. The experts also considered fertility in their discussion of disease recurrence in the podcast.
These new guidelines represent a milestone for GTD care, paving the way for better support and outcomes for patients worldwide. Listen to the full podcast with Professor Seckl and Dr Lok here.

Create a lasting tribute to a loved one with a CTRT In Memory page.
Are you thinking of setting up an In Memory page for a loved one on behalf of CTRT but unsure on where to start? We’ve laid out all the information here that you will initially need to create your tribute page.
What is an In Memory page?
An In-Memory is a personalised tribute page that commemorates and celebrates the life of someone special and helps continue raising funds in their memory.
It is an online space where you, your family and friends can share photos, stories, and memories about a loved one and donate to support The Cancer Treatment and Research Trust.
Why create an In Memory page?
An In Memory page is a wonderful way to remember a loved one, to celebrate their life and their commitment to a cause. The funds raised will be used by our charity to conduct life-changing cancer research and support the treatment of patients at Mount Vernon Cancer Centre, Charing Cross, and Hammersmith Hospitals.
Your In Memory page can also be an effective way of keeping track of past, current and future fundraising, or donations you may receive in memory of your loved one by keeping them all in one place.
How do I create an In Memory page?
It’s easy to get started and create your own In Memory page. Simply visit our dedicated In Memory page on the CTRT website here: Online tribute funds and click ‘Create a Tribute fund’ and follow the step-by-step process. It only takes a few minutes to complete. There is an option to set a fundraising target on the page if you would like to include this.
New In Memory feature – Light a Candle
In Memory pages now have the ability to feature a virtual candle which can be lit by a loved one, along with a donation, to mark a special occasion such as a birthday, anniversary or Christmas, or simply to honour a memory. The Light a Candle feature provides you and your family and friends with the opportunity to share a more personal donation in memory of your loved one, and to continue to return and pay tribute to them for years to come.
Click here to access a demo page to see what an In Memory page layout can look like.
Is there a fee to set up an In Memory page?
Your In Memory page is free to set up.
Can I add Gift Aid to my donation?
Yes. If your gift is eligible, simply tick the Gift Aid box when you make your donation.
Can I add offline donations?
If you have sent donations to us separately in the post or have fundraised for an event on a different platform, there is an option for these amounts to be included and combined in your In Memory page fundraising platform. This is usually best practice so that you, your family and friends can see all fundraising in one place.
Is there someone I can talk to directly about my In Memory page?
If you have any questions or want to chat through setting up your page, the friendly CTRT can help. Please contact us by email on info@ctrtrust.co.uk or give us a call on 07758 739185.
Thank you for considering setting up an In Memory page to honour the memory of your loved one and support CTRT in our important cancer research.
Set up your In Memory page with CTRT here: Online tribute funds













